Can sleep apnea cause pain? – What we know and 19 practical remedies
By Jason Wooden, PhD | August 1, 2021
If you’re curious whether sleep apnea can cause pain, two things happen in the body that affect pain. Sleep apnea patients sleep more poorly which can make them more sensitive to pain and sleep apnea may trigger more inflammation in the body.
The good news is that there’s plenty of things you can do – better sleep hygiene, sleep apnea treatment, pain meds, medical procedures, physical therapy, dietary changes, exercise, massage, and a variety of natural remedies.
Why it’s not so crazy you’re curious whether sleep apnea can cause pain
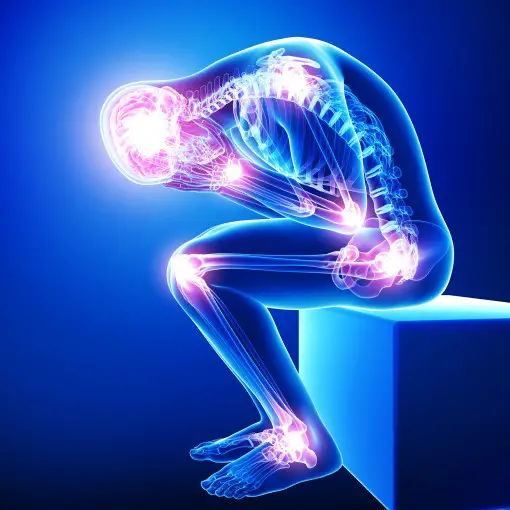
Given what pain does to us, it’s understandable if you’re wondering whether sleep apnea can cause pain and body aches.
Pain makes it harder to do everyday tasks, concentrate, move around, socialize, sleep, and enjoy everyday life.

It’s natural to want to avoid anything that can trigger or worsen pain symptoms.
With more than 22 million people living with sleep apnea in the US and nearly a billion worldwide, you’re likely not the only one wondering about sleep apnea and pain.
Whether you’ve recently had a pain flare or ongoing pain that lately seems to be worse, it’s fair to ask if there’s connection given all the other things sleep apnea does to the body.
Obstructive sleep apnea, the most common type, occurs when muscles in the throat relax during sleep. This causes the airway to collapse, breathing pauses throughout the night, and loud snoring.
It’s been linked to all sorts of things – an increased risk for high blood pressure, heart disease, stroke, heart attacks, diabetes, and depression.
That’s a lot of stuff…
So, it’s not so crazy you’re curious whether obstructive sleep apnea can cause pain too.
Pain is a signal from your body telling you something may be wrong…
It can be acute (sudden) or chronic (ongoing.)
Among the known causes for pain are:
- injury or trauma to the body
- headaches or migraines
- infections
- diseases such as cancer and heart attacks
- inflammatory conditions such as arthritis, asthma, or gout
- nerve damage
- depression
Should sleep apnea be on the list of suspects for your pain?
Let’s take a look at what could be happening and what you can do about it.
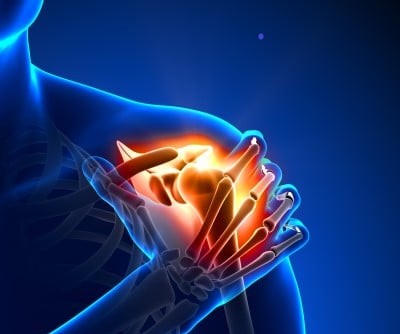
Can sleep apnea really cause pain?
For starters, there’s definitely an association between sleep apnea and chronic pain.
Would you believe studies have found that 55 percent of obstructive sleep apnea patients also experience chronic pain? Whether it’s a direct or indirect connection, it’s hard to say.
Nonetheless, two things are going on in people with obstructive sleep apnea that are known to affect pain:
You’re sleeping more poorly
If your sleep apnea is not under control, you’re not sleeping as well. Researchers have found that insufficient sleep, fragmented sleep, or poor sleep quality can lower your pain tolerance.
This will cause you to be more sensitive to body aches and pain.
There’s more inflammation in the body
Inflammation is important for protecting and healing the body. Unfortunately, one of the things it also does is to turn on pain signals.
Recent research has revealed that sleep apnea causes low grade inflammation in the body. The extra inflammation could aggravate any pain issues you already have.
So, that’s what sleep apnea could do to pain – cause a flare up of something minor or aggravate ongoing pain and body aches.
And that’s why it may seem like sleep apnea is causing pain.

The vicious link between sleep, sleep apnea, and pain
So, far we’ve talked about how sleep apnea could cause pain. However, we all know how bad pain is for sleep.
In the US, over 100 million people suffer from chronic pain. It’s no surprise that 70 percent of them have trouble sleeping.
Why is pain so hard on us at night?
First off, pain makes it harder to relax and fall asleep.
Secondly, it can also cause you to wake up more during the night as you toss and turn to get more comfortable.
If you’re not careful, you can get into a vicious cycle since poor sleep can increase your sensitivity to pain – poor sleep leads to more pain and pain leads to poorer sleep.

What about sleep apnea and headaches?
So, what’s up with the morning headaches some people with sleep apnea get?
Researchers are still figuring this out but one thing they think could be going on in sleep apnea patients relates to the buildup of carbon dioxide in the body.
Basically, as your breathing is repeatedly interrupted during the night, air gets trapped in lung. As a result, carbon dioxide builds up in the blood stream causing blood vessels in the brain to dilate.
And dilation is what gives you a headache.

Other things you that can make your pain worse
Obviously, sleep apnea isn’t the only thing that can aggravate pain symptoms.
In fact, there are lots of things you do every day that could be making things worse.
Some of things to think about are:
Inactivity – A sedentary lifestyle can increase your risk for chronic pain.
Junk food – Some of your favorite foods and snacks unfortunately can cause inflammation and aggravate your pain. This includes dairy, nightshade vegetables, processed meats, sugar, and other refined carbs.
Stress – Feeling stressed out can trigger the body’s “fight-or-fight” response which can cause more inflammation and aggravate pain. Learn more
Smoking – It may bring short-term relief, but over the long-term worsen pain. Nicotine can slow healing and cause degeneration in parts of the body. Learn more

19 Things you can do to keep your pain more manageable
If you’re worried that sleep apnea may be worsening your pain, the good news is that there’s plenty of things you can do for pain management.
And if you keep your pain more manageable, that will help keep you out of the cycle of pain and poor sleep.
1) Sleep
Given how much sleep affects pain, it should be no surprise it’s at the top of the list.
It’s important you’re making the best of your sleep opportunities. Do what ever you can to get as much as quality rest as possible.
Start with sticking with your sleep hygiene and doing everything you can to keep your sleep on schedule. Your every day habits can set the stage for deep restful sleep.
Poor sleep hygiene can sabotage everything else you’re doing to improve your sleep. (What good is it if your sleep apnea treatment is working but you’re up into the wee hours of the morning because you’re drinking too much cola?)
For better sleep hygiene, sleep experts suggest you:
– keep consistent wake up & sleep times
– avoid naps
– exercise during the day
– avoid large meals, alcohol, or stimulants such as caffeine before bedtime
– maintain a regular bedtime routine
– avoid using TVs, laptops, or other electronics before sleep
– keep your bedroom dark, cool, quiet, & relaxing
2) Sleep apnea treatment
If you want to sleep better, you of course have to get your sleep apnea under control.
You should also make sure you have a sleep apnea treatment that’s working for you. Some people have a hard time with CPAP, the most common obstructive sleep apnea treatment, and give up.
That’s for sure to keep you in the cycle of pain and poor sleep.
Today, there are plenty of options to pick from including positioning devices, innovative neural therapies, and surgical implants.
Learn more:
Sleep apnea diagnosis
The latest CPAP alternatives
3) Pain meds
Your options include popular over the counter relievers such as acetaminophen (Tylenol) and ibuprofen (Advil). There are also powerful prescription painkillers such as codeine, morphine, oxycodone, and Vicodin.
5) Try heat
Heat can relax muscles and open up blood vessels. This can help the body’s healing process and provide some pain relief.
You can try a warm shower or a heat pack.
7) Check your ergonomics
Humans aren’t designed to sit in front of a desk and computer 8 hours a day. The result is injuries to the shoulder, wrist, elbows, neck, back and hands.
Make sure you have an ergonomic setup. Learn more
Likewise, if you’re doing heavy lifting or other repetitive tasks make sure you’re doing it properly. Learn more
8) Watch your posture
Poor posture can place stress on the spine and lead to back pain. Pay more attention to how you sit, walk, and lift objects. Learn more
9) Improve your bed support
An old “out of shape” mattress can lead to more aches and pains. Find a mattress that works better for your body type and the way you sleep.
A couple websites that review mattresses:
Best mattresses based on in-depth reviews (ConsumersAdvocate.org)
10) Physical therapy
Physical therapy is good for strengthening muscles and increasing flexibility which can help keep you from aggravating old injuries and getting new ones.
It’ll also increase blood flow and reprogram your nervous system to make it less sensitive to pain.
11) Exercise
Contrary to what you may think, studies have found exercise can help people manage their pain. Low impact and gentle activities such as walking or swimming can help improve your pain threshold.
Exercise will also help your sleep apnea and sleep.
Depending on how serious your pain situation is, it’s worth checking with a doctor about the best activities for you.
13) Therapeutic massage
Massage therapy helps relieve pain through relaxing painful muscles and joints, reducing stress and anxiety, and overriding pain signals.
14) Acupuncture
Acupuncture is derived from traditional Chinese medicine, developed over a period of more than 2000 years. It works by stimulating specific points on the body with thin needles.
It’s been shown to be useful for a wide variety of ailments including pain.
15) Psychotherapy
Did you know that pain has biological, psychological, and emotional factors?
Psychotherapy can change the way you cope with their pain and change the stress response in the brain responsible for the release of chemicals that make pain worse.
16) Music therapy
Studies have shown that music can promote relaxation and help relieve pain. It alleviates anxiety and stress which can contribute to pain.
17) Tai chi
Studies have shown Tai chi can help people manage pain. It uses breath control, meditation, and gentle movements to stretch and strengthen muscles.
It can also relax the body and reduce stress.
18) Yoga
Similar to Tai chi, yoga uses breathing, meditation, and stretching. It calms the body and mind which can help reduce stress that triggers pain.
19) Meditation
Meditation can be used to calm the mind and the body. It helps reduce the stress response.
Why it’s really worth getting a checkup
Getting your sleep apnea under control can help with your sleep and pain.
However, it still worth getting a checkup, especially if poor sleep and pain has become a fact of life.
First off, a doctor can check for other health issues linked to poor sleep. The list includes asthma, diabetes, heart disease, and mood disorders.
Secondly, they can check for other things that may be worsening your pain.
According to the US National Institutes of Health, you should seek medical help if:
- shoulder pain with a fever, swelling, or redness
- problems moving the shoulder
- pain for more than 2 to 4 weeks, even after home treatment
- swelling of the shoulder
- red or blue color of the skin of the shoulder area
A doctor can order special tests to help figure out what’s going on.
Useful links:
All about pain (NIH)
Non-opioid options for managing pain (Harvard Health)
How to Treat Fibromyalgia (Healthline)
How to Get off Pain Pills (American Addiction Centers)
You may also be interested in:
3 Ways sleep can help the pain go away
How to improve your sleep hygiene
12 of the latest sleep apnea treatments
Turmeric curcumin for pain and sleep
What to do if shoulder pain is keeping you from sleeping on your side
What you can try if CPAP isn’t working for you
Sources:
1. “Sleep apnea information for clinicians”, American Sleep Apnea Association website
2. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis, Lancet Respir Med. 2019 Aug; 7(8): 687–698.
3. Sleep Apnea Information Page, NIH website
4. Chronic Pain, MedlinePlus
5. “Chronic Pain”, Familydoctor.org
6. Chronic widespread musculoskeletal pain in patients with obstructive sleep apnea syndrome and the relationship between sleep disorder and pain level, quality of life, and disability, J Phys Ther Sci. 2015 Sep; 27(9): 2951–2954.
7. “The Association of Obstructive Sleep Apnea and Chronic Pain”, MedScape
https://www.medscape.com/viewarticle/804588
8. “Inflammatory Pain”, Springer Nature website
9. Obstructive sleep apnea linked to inflammation, organ dysfunction, 2019, ScienceDaily
10. “Sleep and Pain: How Pain Contributes to Sleep Loss”, 2019, Alaska Sleep Clinic website
11. Breaking the Cycle of Chronic Pain and Disturbed Sleep, Neurology Reviews. 2014 August;22(8):30
12. “The Link Between Headaches and Sleep Apnea”, Florida Dental Sleep Disorders website
Connect with us:
About Us
Better Sleep Simplified® was founded as a place for you to get clear and well-researched information.
Our goal is to make sure you know about your options so that you take action sooner rather than later.
Check us out on YouTube:
Watch and Learn
Helpful sleep tips, interesting sleep facts and statistics you want to know about
Affiliate Disclosure
This site is a participant in the Amazon Services LLC Associates Program and other affiliate advertising programs designed to provide a means for sites to earn advertising fees by advertising and linking to them.
Important: BetterSleepSimplified.com is for informational purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis, or treatment. Always consult a physician for sleep and health concerns. See additional information.
